Background
Somalis globally suffer from mental health problems at a higher rate – 1 in 3 – compared to the general population. According to the United Nations Refugee Agency, Somali refugees and asylum seekers comprise one of the fastest growing populations seeking international amnesty (UNICEF, 2018). A study by Onyut et al. (2009) showed that 48.1% of Somali refugees had Post Traumatic Stress Disorder. Somalis did not come as refugees to the UK until the 1980s but migration started as early as the late 1800s from British Protectorate Somaliland (Hammond, 2013).
There are no words for depression in Somali language and there are no diagnostics terms nor ‘personality disorders’ little awareness of mental health illness. Stigma is huge amongst Somalis and in the motherland people with serious mental illness are locked up or chained up. The perception is that you are either “sane” or “crazy” with a view of no o little recovery. First contact would be spiritual healers as people might be believed to be possessed by Jinns (spirits). There is a fear of being “injected” and becoming like a “zombie”.
Adjusting into individualised Western societies from often society orientated nomadic backgrounds, difficulty finding jobs, racism, increasing risk of depression in Somali refugees from London (Mohamud et al., 2004). A study by Bhui et al. (2006) found a 33.8% prevalence rate of depression, anxiety and PTSD in 143 Somali refugees living in the UK. Psychological symptoms are expressed as somatic symptoms such as headaches, body aches, lack of energy, back pain, arthritis, abdominal pain and gastrointestinal problems, insomnia or unusual symptoms that are not described in the DSM (Bhui et al., 2003; Carroll et al., (2004). Conflicting evidence has also suggested there might be a link between the use of the stimulant khat (common for Somalis) and mental health problems (Bhui et al., 2016; Bhui and Warfa., 2010).
Stimulant khat use is common within Somalis and can increase risks in mental health problems (Bhui et al., 2016) although previous study has shown low level psychotic symptoms with its use (Bhui and Warfa, 2010). Even though it is illegal to use since 2014 in the UK and classed as class C drug, which can turn Somalis to more dangerous use of drugs.
Factors that may contribute to the increased risk of depression in Somali refugees include adjusting into individualised Western societies from often society-orientated nomadic backgrounds, difficulty finding jobs and racism (Mohamud et al., 2004). Other contributing factors include intergenerational traumas, war, genocide, displacement, negative emotions not openly discussed, identity crisis, discrimination, Islamophobia, socio-economic factors, stigma, housing, vitamin D deficiency, vulnerability due to language problems and lack of advocacy, loss of extended family and support, and hidden alcohol problems with lack of culturally sensitive drug and alcohol services, intergenerational gap, Female Genital Mutilation/Circumcision, facing new problems of grooming into gangs, and additional responsibilities of sending remittances abroad to
family and worries of extended families due to risks of war, insecurity, poor health services, environmental vulnerability e.g. floods or droughts destroying crops and livestock.
Study by Palmer (2006) has shown Somali communities in Camden reported mistrust of the system, fear, cultural barriers, anxiety over immigration status and access to housing. Poor treatment of Black people within mental health services has been highlighted greatly by Akther (2019). Black people were most likely to be involuntarily admitted and readmitted to hospital compared to White people partially due to an increased perceived risk of violence. Memon et al. (2016) reported that BME participants perceived power imbalance and that White British GPs and specialists were unable to understand or sympathise with the realities and experiences of those from a BME background. Cordoba (2020) stresses the importance of person-centred approach in psychiatry education and practices, where patients are empowered in shared-decision making, co-production or collaborative care using ethics, community engagement or social inclusion complemented by values of communication, dignity, empathy, fairness, honesty, humility, respect and trust (Cordoba, 2020).
Somali women have previously reported feeling stigmatised and retraumatised in accessing healthcare services thus creating barriers in trust, delays of treatment and looking for alternative sources (Karlsen et al., (2020).
A recent paper by Linney et al. (2020) aimed to understand the views of Somalis living in Bristol on the causes of and treatment for mental illness, access to services, barriers, cultural factors and how to improve services due to concerns about a recent increase of suicide rates in the close-knit community. Studies have shown worldwide that Somalis have higher rates of mental illness problems and very low access rate.
Caption: 48.1% of Somali refugees meeting the criteria for Post-Traumatic Stress Disorder.
Methods
The authors utilised a community-based participatory research (CBPR) approach which involves working collaboratively with community organisations to conduct studies. CBPR is a collaborative partnership with the communities and researchers have equal say in process, decision making and ownership. The benefits of such approach are to have better understanding and knowledge to influence interventions and policies. CBPR emphasises mutual respect, co-learning between researchers and community members where lived experience, knowledge, understanding and wisdom is shared.
Qualitative focus groups were used to collect opinions and experience from members of the local Somali community on their understanding of mental health including knowledge, culture, causes, treatment, access and improvement to services. The
researchers asked questions about the impact and in relation to men, women and young people.
There were 4 researchers who conducted the focus groups – two of whom were Somali male researchers from two different local Somali organisations, two female primary researchers and three female qualitative methodology experts from Bristol University. The researchers were approached by the Somali community due to increase of suicidal deaths amongst Somalis.
Recruitment was through word of mouth and advertising of information sheets in both Somali and English. To increase variety in participation, the Somali researchers asked individuals at the community centres if they would participate and/or knew any anyone else willing to take part.
Four focus groups separated by gender were held with 5-6 people per group. The majority of participants were parents and their ages ranged from the late 20s to 60s with majority participants aged between 30 and 45. All participants were given anonymous numerical codes due to the closeness of the community. Open ended questions were asked and the data were analysed using thematic analysis with use of NVivo software for data management, The participants had been living in Bristol between less than a year to over 20 years and had a wide range of verbal English language skills, from very basic to advanced/ fluent.
The focus groups were run by both female primary researchers with the same male Somali interpreter always present to provide continuous Somali to English translations throughout. Most participants spoke in Somali and English-speaking participants confirmed the translation has been correct to the researchers. The focus groups lasted between 33 and 50 minutes.
Results
A total of 23 participants (12 male and 11 female) were recruited. The four focus groups which took place over one month yielded four themes: knowledge of mental illness; culture; ideas for improvements; and access to healthcare.
There were interestingly differences in opinions of what causes and contributes to mental illnesses from Somali men and women. Men identified socio-economic factors such as poverty, unemployment and homelessness, trauma, language barrier between mother and child, and family separation and conflict. Women however focused more on
family dynamics, lack of sleep from children not coming home, gender roles, the belief of heritable risk factors in children, and young people not recognising mental illness. Somali women reported physical symptoms of mental illness, and both men and women spoke of the fear of community gossip leading to isolation exacerbated due to stigma.
Participants also spoke of the effects of the trauma from the Civil War in Somalia on the mental health of Somalis in the UK and the cultural disconnect from settling in the UK.
Female participants identified preference of use of spiritual healing as treatment such as reading the Qur’an, along with medication and talking to others. Whilst men also listed religious healing and medication, they further mentioned going “back home”.
Some of the factors affecting accessing services included language barriers, long waiting times, lack of continuity in clinicians, lack of flexibility of interpreters when needed and not knowing where to access appropriate services. Somali men further noted their lack of trust of professionals lack of mental health awareness in the community in the UK and back home, no community facilities for young people and homelessness.
From young people’s perspective Somali adults acknowledged that there was an intergenerational gap, communication barriers, lack of awareness and hardly any social activities in the community which has an impact on their mental health.
Although there was black and white thinking of either being classified as “crazy” or “sane” with no grey areas, participants recognised increased support in the community would help improve health inequalities. Solutions by the community were having interpreters on standby, more information awareness and support, triage system in the community and having elder Somalis as representatives or link workers. Interesting no self-disclosures were given in the focus groups.
Conclusions
This study found key differences in Somali views on mental illnesses which may differ from mainstream views including the reporting of somatic symptoms as a sign of mental ill health.
The authors concluded that it has founded new evidence that that some Somali women explained that mental illness problems started with the physical symptom such as headaches is a new finding and has not been described in previous studies. Another new finding was attributing causes of mental illness in children as heritable or belief that younger siblings can inhibit their behaviour. Although researchers acknowledged that this could be due to heritable nature autism which there have been increased campaigns in Bristol.
Low access rates attributed to a lack of knowledge of mental ill health, stigma and general limitation in access to healthcare. It was suggested this could be improved through community initiatives, English education, culturally safe services, rapport and trust building, raising awareness and the use of health link workers.
Strengths and limitations
· The research study has been very thorough and reflected on many issues that have been reported before in previous research. There was good selective systemic review explaining the background, trauma and socioeconomical factors. It highlighted well that participants are aware of problems and knowing the solutions. This research is unique as the Somali community approached the researchers first and demonstrated very good collaborative working throughout.
· There has been good collaboration through the use of community based participatory research focusing on the unique strength of the Somali communities to enhance understanding. Open questions allowed for flexibility and story telling which Somalis are known for. Collaboratively working from the participants and researchers throughout the process.
· Two researchers were of Somali descent of the same city however both were male. It would have been better to have atleast one female Somali researcher who could have invoked more openness in the two female focus groups. Lead researchers being non-Somalis which could help in high levels of stigma community with more openness and trust. The fact that has been some previous partnership work recently also improved trust.
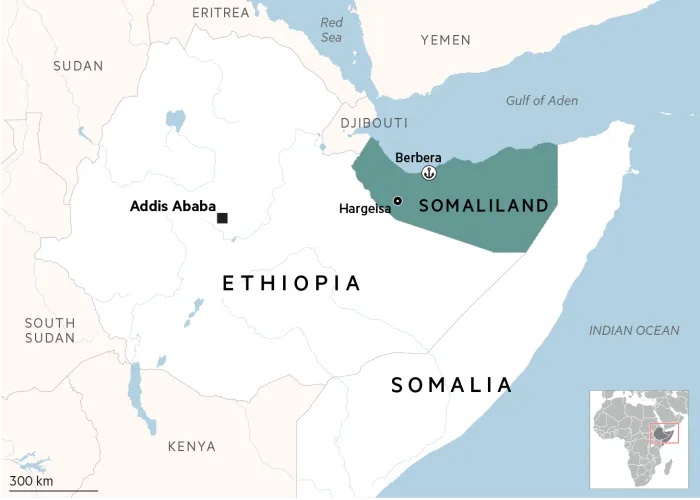
· There was no mention of intertribal issues and racism that could arise from participants in the same group and researchers. Tribe belonging is part of identity as Somali culture is based on a clan-based social system that emphases patriarchal lineage and wider family bonding. Somali society is comprised of several major clans which subdivided into further sub clans. A civil war and genocide happened due to dictatorship, tribal nepotism and discrimination toward others clans which included genocide and bombing of entire Hargeisa city. Since 1991 Somalia has not seen democratically elected government and interclan conflicts are continuing to happen unlike Somaliland which reclaimed its independence and been peaceful since 1991. Belonging to a clan plays more of importance than belonging to wider Somali society (Jacob et al., 2018)
· There was no breakdown of housing status and having lived in other countries or immigrations if they were from Djibouti, Somaliland, Somalia, Somali regions of Ethiopia or Kenya, Europe or Arab countries etc. The current study was small and carried out in Bristol, so this data represents the views of participants in one geographic area, as most participants lived in one neighbourhood.
· A strength was to disseminate information face to face rather than leaflets as a lot of Somalis are an oral story telling community. The use of one translator throughout was good however it would have been better if the translator was female due to sensitivity.
· Focus groups were held in the community centre however it could have been enhanced if one to one session or telephone consultations took place due to fear of stigma and confidentiality in close knit community. There could have been better results due to the sensitivity and stigma if one to one interviews were conducted with the option of telephone interviewing. This would also eliminate
any influential person (such as a community leader) that wasn’t challenged in the group settings and disclosures of lived experiences stories.
This is reflected on no disclosed lived experience in all focus groups nor as carers and family except for one in the latter group. The study did not involve Somali people with lived experience nor any family/carers input.
There was a diverse sample was sought in terms of age, gender, time living in Bristol, number of children, and English language ability but no youth involved.
· Systemic literature review highlighted showed outdated research and conducted in Somali refugees not first and second generations of Somalis. This proves the need for further research needed in the Somali community and global patterns of low access rates.
· The study claims to find a new finding of reporting of headaches by female participants however study by Carroll et al. (2004) did describe Somali participants reporting headaches and other physical health symptoms part of experiencing sadness or suffering which connoted to the Somali ‘murug’.
· This study doesn’t address institutional racism within the NHS nor education of transcultural psychiatry within education and organisations and their need to be equipped to be culturally sensitive in order to be fit to help Somalis clients. The study mentioned Somalis were hard to reach which is quite a patronising term as participants’ feedback makes it clear it is actually services that are hard to reach.
· There was no wider acknowledgement of traumas caused by Female Genital Mutilation/c, Islamophobia, discrimination, institutional racism, profiling at airports, health settings and schools, vulnerability of grooming and gangs, socio-economic factors, racism, additional burden and stress of sending remittance to relatives abroad and continued worries of risks of intertribal, terrorism, environmental disasters affecting relatives in the motherland. Researchers could have asked direct questions on tribes and FGM on impact on mental health to generate discussion due to sensitivity or give the option to give feedback separately or on paper.
· The views of Somali adolescence were not asked and only their parents which could not give full picture due to stigma nor highlight the impact of growing up in two cultures.
· No participants were interviewed with lived experience or their carers which could have given a better result thus solutions.
Implications for Practice
· In my clinical practice I have witnessed positive effects when looking after Somali clients as they did not speak English nor t understood their section. By providing psychological safety and person- centred care, I was able to help,
advocate and signpost to appropriate services whilst reassurance given to extended family members that their loved ones were not alone. Translators are often only provided during weekly medical reviews so it can be a daunting and lonely place if you are brought to hospital against will, medicated and unable to leave until you are reviewed by a Psychiatrist. So for example ability to order halal meals or escorting to halal restaurants are little perks when they are not used to hospital food. I remember once being told that a Somali patient were described as doing “unusual activities” washing feet in the sink not knowing the person was performing ablution.
· Privacy is important especially for females who often wear headscarf and being in presence on mixed ward can create further inequality especially when you do not speak the English language well and face difficulty performing prayers or have access to the Qur’an audio or Holy Book. Especially during pandemic, it was challenging when family visits were limited and no children are allowed inside. Despite having higher problems, high levels of stigma and low level of access, there are not many Somali mental health professionals in the field which should be promoted and increased.
· There is a phrase used in the community to describe the “dulling” effect of psychiatric medication on a person’s expression. It is said that that person “got injected”. There is a common belief that once you are mentally unwell being a life sentence.
· There are no words for depression in Somali language nor diagnostic terms like ‘personality disorders’ and there is little awareness of mental health illness. Stigma is widespread amongst Somalis and in the motherland where it is not uncommon for mentally ill people are locked and chained up.
· Services aren’t equipped to deal with needs of Somalis and there is a lack of Somali mental health professionals and therapists in the UK. Often Somalis come in contact with mental health services at crisis point and early intervention through the community should be implemented.
· Assistance and advice with practical issues such as housing, immigration, benefits and access to employment and training opportunities can be a crucial supportive intervention when dealing with a group who are dealing with the pressures and anxieties of living in exile.
· A successful case study is Hayaan Project, part of Mind in Harrow which provides holistic and culturally sensitive approach and advocacy to people and their family members. Fortnightly sessions are held by Somali psychodynamic counsellor Abdi Gure and retired Somali Consultant Psychiatrist and Professor Dr Fido in Somali language educating about different topics in mental health. Advocacy is provided in the community and inpatient wards, closely working with extended family, advice and signposting. Volunteers and peers support
workers are trained on a yearly basis to continue help with outreach work. Local organisations, charities and NHS Trusts work closely with Hayaan and come in as guest presenters (Changemakers, 2015).
· A Seattle-area pilot project called “Islahul Qulub: Islamic Trauma Healing” combines prayer, prophet narratives, and guided discussion in a six-week PTSD intervention program tailored for Somalis suffering in the aftermath of war-torn conflict.
· What would likely be considered severe psychopathology in Western cultures may be described as a consequence of jinn from a traditional Somali perspective (Elmi, 1999). Jinn are spirits that possess supernatural powers capable of entirely controlling human processes, including psychological processes (Carroll, 2004). Symptoms may include visual or auditory hallucinations, speaking in tongues, not eating or sleeping, and general lack of interest in life’s activities.
· This research has also highlighted the importance of further research should be held especially primarily lead by Somali researchers to incorporate better beliefs and practices in health care in health services (Leininger et al, 2006).
· Study done by Wolf et al (2016) acknowledged the importance of traumas, availability of translators, extended visiting hours, negative effects of khat use, inclusivity of extended family members and importance of having Somali healthcare staff to reduce health inequalities. Interpreters and Somali professionals should be trained in mental health awareness and if preferably translators to be employed by Trusts Bank systems for consistency, reliability and continued training.
· Collaboratively working with spiritual healers, imams in mosques who can refer people on is important including continues psychoeducation in the community and NHS organisations. Somali people are natural story tellers and the use of art in Somali are alternative ways becoming more inclusive integrated working. Social workers who could help with social aspect in mental health recovery are often feared wrongly with fear of removal of children however with psycho education and employing more Somali staff this could be prevented. Specialist services community centred and culturally and spirituality sensitive. Service providers becoming anti-racist and implement trauma informed practices and interventions.
Statement of interests
I am of Somali background working in mental health services who has lived majority of my life in the EU and my family have fled the country before the civil war so my interpretation may be biased.
Links
Primary paper Linney, C., Ye, S., Redwood, S., Mohamed, A., Abdullahi, F., Biddle, L. and Crawley, E. (2020).. “Crazy person is crazy person. It doesn’t differentiate”: an exploration into Somali views of mental health and access to healthcare in an established UK Somali community. International Journal for Equity in Health. 19, 190. DOI:https://doi.org/10.1186/s12939-020-01295-0
Other references
Akther, S.(2019). Racial disparities in bipolar disorder diagnosis and treatment: time to talk about racism. The Mental Elf [online] May 03. 2019.
Bhui, K. andWarfa. N. (2010). Trauma, khat and common psychotic symptoms among Somali immigrants: a quantitative study. Journal of Ethnopharmacology,132(3), 549–53. DOI: 10.1016/j.jep.2010.07.027
Bhui, K., Abdi, A., Abdi, M., Pereira, S., Dualeh, M., Robertson, D., Sathyamoorthy G., and Ismail H. (2003). Traumatic events, migration characteristics and psychiatric symptoms among Somali refugees–preliminary communication. Soc Psychiatry Psychiatr Epidemiol, 38(1), 35-43. DOI: 10.1007/s00127-003-0596-5. PMID: 12563557.
Bhui, K., Craig, T., Mohamud, S., Warfa, N., Stansfeld, S. A., Thornicroft, G., Curtis S. and McCrone P.. (2006). Mental disorders among Somali refugees: developing culturally appropriate measures and assessing socio-cultural risk factors. Soc Psychiatry Psychiatr Epidemiol, 41(5), 400-408. DOI: 10.1007/s00127-006-0043-5.
Carroll, J.K. (2004). Murug, Waali and Gini: Expressions of Distress in Refugees From Somalia. Primary care companion to the Journal of clinical psychiatry, 6 (3), 119–25. https://doi.org/10.4088/pcc.v06n0303
Cordoba, E. L.(2020) Person-centred care: challenges and changes to the training of psychiatrists. The Mental Elf. [Online] December 23, 2020.
Hammond, L.(2013). Somali transnational activism and integration in the UK: mutually supporting strategies. Journal of Ethnic Migration Studies, 39(6),1001–17. DOI: 10.1080/1369183X.2013.765666
Karlsen, S., Carver, N., Mogilnicka, M. and Pantazis, C. (2020).
‘Putting salt on the wound’: a qualitative study of the impact of FGM-safeguarding in healthcare settings on people with a British Somali heritage living in Bristol, UK.
BMJ Open, 10:e035039. DOI: 10.1136/bmjopen-2019-035039
Leininger, M. M., McFarland, M. R. (2006). Culture care diversity and universality: A worldwide nursing theory. Sudbury, MA: Jones & Bartlett.
Mental Health Is Not Taboo. Changemakers website. Last accessed 20 Nov 2020.
Memon, A., Taylor, K., Mohebati. L.M., Sundin, J., Cooper, M., Scanlon, T. and Visser, R.D. (2016). Perceived barriers to accessing mental health services among black and minority ethnic (BME) communities: a qualitative study in Southeast England. BMJ Open, 6:e012337. DOI:10.1136/bmjopen-2016- 012337
Mohamud, S., Bhui, K., Craig, T., Warfa, N., Stansfeld, S., Curtis, S., et al. (2004). Residential mobility and mental health: A cross-sectional study of Somali refugees in London. Ethnicity & Health, 9, S80-S81.
Onyut, L.P., Neuner, F., Ertl, V., Schauer, E., Odenwald, M. andElbert, T. (2009). Trauma, poverty and mental health among Somali and Rwandese refugees living in an African refugee settlement – an epidemiological study. Conflict and Health, 3(6). DOI: 10.1186/1752-1505-3-6
Palmer, D. (2006) Imperfect prescription: mental health perceptions, experiences and challenges faced by the Somali community in the London Borough of Camden and service responses to them. Primary Care Mental Health, 4(1), 45– 56. Google Scholar.
The United Nations Refugee Agency (2018). Accessed 22 Nov2020 from https://www.unhcr.org/somalia.html.
Wolf, K.M., Zoucha, R., McFarland, M., Salman, K., Dagne, A. and Hashi N. (2016). Somali Immigrant Perceptions of Mental Health and Illness: An Ethnonursing Study. Journal of Transcultural Nursing,27(4),349-358. DOI:10.1177/1043659614550487.
Categories: Opinion